Gentle Strategies to Help an Infant with Reflux
Infant reflux can be a frustrating and exhausting experience—for both babies and their caregivers. That telltale spit-up, the arched back, the cries during or after feeds—it’s heartbreaking to watch and can make feeding feel stressful. The good news? Reflux is common and usually improves with time, and there are plenty of gentle, supportive ways to ease your baby’s discomfort in the meantime.
Here are some strategies that can help manage infant reflux naturally and effectively:
1. Feed in an Upright Position
Keeping your baby’s body more vertical during and after feeds can make a big difference. Try holding your baby at a 45-degree angle (or more upright if they’re comfortable) while feeding. After the feed, continue holding them upright for 20–30 minutes to help gravity keep milk down.
2. Smaller, More Frequent Feeds
Overfilling your baby’s tummy can contribute to reflux. Instead of spacing out large feeds, try offering smaller amounts more often. This can reduce the pressure on their tiny stomachs and give them a chance to digest more comfortably.
3. Watch for Feeding Cues and Avoid Overfeeding
Feeding on cue—when your baby shows early signs of hunger like rooting or sucking on their hands—helps ensure they’re not too hungry or too full, both of which can increase reflux episodes. Try not to force a full feed if your baby is signaling they’re done.
4. Check for a Shallow Latch or Feeding Difficulties
Sometimes, reflux-like symptoms are linked to feeding mechanics. A shallow latch can cause your baby to swallow more air, increasing spit-up and gas. A tongue tie could also be a factor. A lactation consultant can assess latch and feeding dynamics, whether you’re breastfeeding, bottle-feeding, or doing both.
5. Burp Frequently
Burping during and after feeds can help release trapped air. Try burping your baby every few minutes during a feed, and experiment with different burping positions—over the shoulder, seated with back support, or tummy-down across your lap.
6. Reevaluate Bottle and Nipple Flow
For bottle-fed babies, the type of bottle and nipple flow can have a big impact. A flow that’s too fast can lead to gulping and more air intake, while a flow that’s too slow might cause frustration and more swallowing of air. Look for paced-feeding techniques and bottle options designed to reduce air intake. The Lansinoh bottles are a favorite of mine.
7. Use Tummy Time Mindfully
Tummy time is important for development, but it can be uncomfortable for babies with reflux, especially right after a feed. Try tummy time when your baby’s stomach is emptier—before a feed or a while after digesting—to avoid pressure on their belly.
8. Try Gentle Movement
Some babies with reflux are comforted by gentle rocking or babywearing. Upright baby carriers can keep your baby close and supported while helping reduce reflux symptoms. Make sure their airway is always clear and their chin isn’t resting on their chest.
9. Explore Bodywork Options
Tension in the body can impact digestion and feeding. Gentle therapies like infant craniosacral therapy or pediatric chiropractic care (with a qualified provider) may help babies who have persistent reflux symptoms related to body tension, birth trauma, or feeding dysfunction.
10. Know When to Seek Medical Guidance
Most infant reflux is mild and improves on its own. But if your baby is losing weight, refusing feeds, crying inconsolably, or has symptoms like projectile vomiting or blood in the stool, check in with your pediatrician. Sometimes medication or further evaluation is necessary.
You’re Not Alone
Reflux can test your patience and make you question your instincts, but you’re doing an incredible job. With the right tools, support, and a little time, most babies outgrow reflux and become happy, comfortable feeders. If you ever feel overwhelmed, reach out—you’re not alone on this journey.
Need extra support with feeding or reflux? I offer gentle, holistic lactation and infant wellness services to help you and your baby thrive.
Maintaining Milk Supply After Returning to Work: A Guide for Breastfeeding Parents
Returning to work after having a baby can be a challenging transition, especially when you’re committed to maintaining your milk supply. Between busy schedules, pumping breaks, and managing stress, it’s easy to feel overwhelmed. However, with the right strategies, you can successfully balance breastfeeding and your career. Here’s how to keep your milk supply strong while working.
1. Establish a Strong Supply Before Returning to Work
The foundation for maintaining your milk supply at work starts before you even go back. In the first few weeks postpartum:
• Nurse frequently and on demand to establish a solid supply.
• Introduce pumping early to build a (small) freezer stash and get comfortable with your pump. You don’t want your last few weeks or days of maternity leave to be spent stressing about having enough milk.
• Consider power pumping if you need to boost supply before your return.
2. Know Your Workplace Rights
The Break Time for Nursing Mothers Law requires many employers to provide time and a private space (not a bathroom) for pumping. Check your company’s lactation policy, and don’t hesitate to advocate for your needs.
3. Stick to a Pumping Schedule
To maintain supply, aim to pump as often as your baby would normally feed. For most parents, this means pumping every 2–3 hours while at work. A typical schedule might look like:
• Pump before leaving for work.
• Pump mid-morning.
• Pump at lunch.
• Pump mid-afternoon.
• Nurse as soon as you’re reunited with your baby.
Consistency is key—skipping sessions can lead to a drop in supply.
4. Optimize Your Pumping Routine
• Use a high-quality pump: A hospital-grade or double electric pump will maximize output.
• Make sure your flanges fit: Ill-fitting flanges can reduce efficiency and cause discomfort.
• Use hands-on pumping: Massage your breasts before and during pumping to increase milk flow.
• Relax while pumping: Looking at photos/videos of your baby or listening to soothing music can help trigger letdown.
5. Stay Hydrated and Nourished
Your body needs extra calories and hydration to keep up with milk production. Keep a water bottle and healthy snacks nearby, and make sure you’re eating balanced meals with plenty of protein, healthy fats, and lactogenic foods like oats, flaxseeds, and almonds.
6. Nurse Often When Home
To reinforce supply, breastfeed frequently in the mornings, evenings, and weekends. Skin-to-skin contact and cluster feeding can help maintain production and strengthen your bond with your baby.
7. Manage Stress and Get Rest
Stress and exhaustion can negatively impact supply. Try to prioritize rest, delegate tasks when possible, and practice relaxation techniques like deep breathing or meditation.
8. Connect with Support
Finding support can make a big difference in your breastfeeding journey. Consider:
• Joining a breastfeeding support group.
• Consulting a lactation professional if you experience supply issues.
• Talking to other working parents for encouragement and tips.
9. Be Flexible and Gentle With Yourself
Breastfeeding while working isn’t always easy, and some days may be harder than others. If you need to supplement with formula or adjust your schedule, that’s okay. The most important thing is your and your baby’s well-being.
By planning ahead, staying consistent, and seeking support, you can successfully maintain your milk supply while working. You’re doing an amazing job—keep going, and trust that you’re providing the best for your baby!
3 Delicious (and easy!) Lactation Treats to Boost Milk Supply
Breastfeeding can be demanding, and nourishing your body with the right foods can help support milk production. These lactation treats are packed with galactagogues—ingredients believed to enhance milk supply—such as oats, flaxseeds, and brewer’s yeast. Plus, they’re easy to make and delicious!
1. No-Bake Lactation Energy Bites
These bite-sized treats are perfect for a quick snack between feedings.
Ingredients:
• 1 cup rolled oats
• ½ cup peanut butter (or almond butter)
• ⅓ cup honey or maple syrup
• ¼ cup ground flaxseeds
• 2 tbsp brewer’s yeast (optional but beneficial)
• ½ cup dark chocolate chips
• 1 tsp vanilla extract
Instructions:
1. In a mixing bowl, combine all ingredients.
2. Stir until fully mixed.
3. Roll into small bite-sized balls and place on a baking sheet.
4. Refrigerate for at least 30 minutes to firm up.
5. Store in an airtight container in the fridge for up to a week.
Tip: Add shredded coconut or chia seeds for extra nutrients!
2. Oatmeal Chocolate Chip Lactation Cookies
These soft, chewy cookies are a tasty way to support your milk supply.
Ingredients:
• 1 cup unsalted butter, softened
• 1 cup brown sugar
• ½ cup white sugar
• 2 eggs
• 1 tsp vanilla extract
• 2 cups rolled oats
• 1 ½ cups whole wheat flour
• 2 tbsp brewer’s yeast
• 2 tbsp ground flaxseeds
• 1 tsp baking soda
• ½ tsp cinnamon
• ½ tsp salt
• 1 cup chocolate chips
Instructions:
1. Preheat oven to 350°F (175°C).
2. In a bowl, cream together butter, brown sugar, and white sugar.
3. Beat in eggs and vanilla.
4. In a separate bowl, whisk together oats, flour, brewer’s yeast, flaxseeds, baking soda, cinnamon, and salt.
5. Gradually add the dry ingredients to the wet ingredients.
6. Stir in chocolate chips.
7. Drop spoonfuls of dough onto a lined baking sheet.
8. Bake for 10–12 minutes or until golden brown.
9. Let cool before enjoying!
Tip: Substitute chocolate chips with dried fruit or nuts for variety.
3. Lactation Smoothie
A quick, nutrient-dense drink perfect for busy moms.
Ingredients:
• 1 cup unsweetened almond milk (or any milk of choice)
• ½ banana
• ¼ cup rolled oats
• 1 tbsp ground flaxseeds
• 1 tbsp brewer’s yeast
• 1 tbsp peanut butter
• ½ tsp cinnamon
• ½ tsp vanilla extract
• 1 tsp honey (optional)
• ½ cup ice cubes
Instructions:
1. Blend all ingredients together until smooth.
2. Pour into a glass and enjoy!
Tip: Add a handful of spinach for extra iron without affecting the flavor.
These treats are great for busy moms who need a nutritious boost while supporting their breastfeeding journey. Want more lactation-friendly recipes? Let me know!
Preventing Bottle Refusal: Tips for a Smooth Transition
Introducing a bottle to your baby can be an emotional and sometimes frustrating experience, especially if they refuse to take it. Whether you’re returning to work, need a break, or just want to share feeding duties, a smooth transition to bottle feeding is essential. The good news is that with patience and the right approach, you can help your baby accept a bottle with ease.
Why Do Babies Refuse Bottles?
Bottle refusal can happen for several reasons, including:
• Preference for Breastfeeding – Babies who are exclusively breastfed may find bottle feeding unfamiliar.
• Timing of Introduction – Waiting too long to introduce a bottle can make it harder for a baby to accept.
• Flow Preference – Some babies struggle with the flow of milk from a bottle, especially if it differs from the breast.
• Feeding Position & Caregiver Differences – Babies may associate feeding with a specific person or position and resist changes.
How to Prevent Bottle Refusal
1. Start Early but Not Too Early
If you plan to introduce a bottle, start around 4–6 weeks old—after breastfeeding is well established but before baby develops strong preferences.
2. Choose the Right Bottle and Nipple
Look for a bottle designed to mimic breastfeeding, with a slow-flow nipple to encourage a similar sucking pattern. You may need to try a few different types before finding one your baby likes.
3. Have Someone Else Offer the Bottle
Babies often associate mom with breastfeeding and may refuse a bottle from her. Try having another caregiver offer the bottle while you are out of the room.
4. Offer the Bottle When Baby Is Calm but Hungry
A very hungry baby may be too frustrated to try something new. Aim for a time when they’re alert but not overly hungry or upset.
5. Use a Breast Milk Scented Cloth
Rubbing the bottle nipple with a cloth that smells like mom or placing it near baby’s face can create a sense of familiarity.
6. Try Different Positions
Some babies prefer to be held in a different position for bottle feeding than for breastfeeding. Try feeding in an upright position or while gently rocking.
7. Maintain Skin-to-Skin Contact
Holding baby close and maintaining skin-to-skin contact can make bottle feeding feel more comforting and natural.
8. Keep It Playful and Low-Pressure
If baby resists, take a break and try again later. Offer the bottle in a relaxed setting without pressure.
9. Experiment with Milk Temperature
Some babies prefer their milk warmer or cooler. Try adjusting the temperature to see what they prefer.
10. Use a Paced Bottle-Feeding Method
Paced feeding mimics breastfeeding by allowing baby to control the flow of milk. Hold the bottle horizontally and let baby suck actively rather than letting milk pour into their mouth.
What If Baby Still Refuses?
If your baby consistently refuses the bottle, stay patient and try different strategies. Sometimes, offering milk in a small open cup, spoon, or syringe can help transition them to bottle feeding. If bottle refusal persists, a lactation consultant can provide additional guidance tailored to your baby’s needs.
With a little time and flexibility, most babies eventually accept the bottle. The key is to stay calm, experiment with different techniques, and trust that your baby will adjust in their own time.
Breastfeeding Positions: Finding the Best Fit for You and Your Baby
Breastfeeding is a beautiful and natural way to nourish your baby, but finding a comfortable position is key to making the experience enjoyable for both of you. The right position can help with latch, prevent discomfort, and support efficient milk transfer. In this guide, we’ll explore different breastfeeding positions, their benefits, and how to find the best one for your needs.
1. Cradle Hold
One of the most common breastfeeding positions, the cradle hold involves holding your baby in your arm, with their head resting in the crook of your elbow.
How to Do It:
• Sit comfortably with good back support.
• Position your baby tummy-to-tummy with you, their head resting on your forearm.
• Support their bottom with your hand while using your free hand to guide their latch.
Best For:
• Full-term babies with good head control
• Relaxed nursing sessions
• Moms who prefer a traditional, close-hold position
Challenges:
• Can be harder for newborns who need more head and neck support
• May put strain on your back and arms if not well-supported
2. Cross-Cradle Hold
Similar to the cradle hold but with more control over the baby’s head, the cross-cradle hold is often recommended for newborns and those learning to latch.
How to Do It:
• Hold your baby across your body, supporting their head and neck with the hand opposite the breast you’re nursing from.
• Your forearm supports their back while your other hand helps guide your breast and their latch.
Best For:
• Newborns and preemies
• Babies struggling with latch
• Moms who need more control over positioning
Challenges:
• Can be tiring on the arms without pillow support
• Requires some coordination
3. Football (Clutch) Hold
This position is great for moms recovering from a C-section or those with twins who need to nurse simultaneously. It keeps the baby’s weight off your abdomen.
How to Do It:
• Tuck your baby under your arm like a football, with their body along your side.
• Use your hand to support their head and guide their latch.
• A pillow can help elevate them for comfort.
Best For:
• C-section recovery
• Moms nursing twins
• Babies who struggle with latch in other positions
Challenges:
• May require pillows for extra support
• Not as commonly used, so may take practice
4. Side-Lying Position
A great option for nighttime feedings, this position allows both mom and baby to rest while nursing.
How to Do It:
• Lie on your side with your baby facing you.
• Support their back with your arm or a rolled-up blanket.
• Latch them onto the breast closest to the bed.
Best For:
• Nighttime or recovery nursing
• Moms with C-section discomfort
• Babies who prefer a more relaxed latch
Challenges:
• Requires careful positioning to ensure a deep latch
• Not ideal for very sleepy babies who may not nurse effectively
5. Laid-Back (Biological Nurturing) Position
This natural, reclined position allows your baby to use their instincts to latch and nurse.
How to Do It:
• Lie back in a reclined position with your baby lying on your chest.
• Allow them to find the breast and latch with minimal guidance.
• Use pillows for extra support if needed.
Best For:
• Encouraging baby-led latching
• Moms with strong letdowns
• Babies who struggle with traditional latching
Challenges:
• May require patience for baby to find the breast
• Not ideal for moms who prefer an upright position
6. Koala Hold (Upright Position)
In this position, your baby sits upright, straddling your lap while nursing.
How to Do It:
• Hold your baby in an upright position, supporting their head and neck.
• Let them latch while sitting on your thigh or supported in a carrier.
Best For:
• Babies with reflux or ear infections
• Older babies who prefer sitting up
• Moms who babywear while nursing
Challenges:
• Requires good head control in younger babies
• May not be comfortable for long nursing sessions
Finding What Works for You
Every baby and mother are different, and the best position is the one that works for both of you. Don’t be afraid to experiment and adjust as your baby grows. Using pillows for support, ensuring a deep latch, and maintaining a relaxed posture can make breastfeeding more comfortable and enjoyable.
If you need help with positioning or latch, working with a lactation consultant can provide personalized support and troubleshooting.
Which breastfeeding position has worked best for you? Share your experiences in the comments!
Do You Really Need the New Munchkin Nipple Shield? Trust Your Instincts Instead
If you don’t need a nipple shield, you don’t need this—trust yourself.
Munchkin recently released a new nipple shield, and while it’s being marketed as a game-changer for breastfeeding moms, let’s take a step back. Do you really need it? More importantly, is it truly helping or just adding another layer of unnecessary intervention to a natural process?
As a lactation consultant, I’ve worked with countless moms who are insecure about their baby’s feeding or their milk supply, and are bombarded with products designed to “fix” breastfeeding when, in reality, their bodies already know what to do. Let’s talk about why nipple shields are often unnecessary and how you can trust your instincts instead.
Why Nipple Shields Exist
Nipple shields can serve a purpose in very specific situations—such as helping premature babies latch or providing temporary relief for severely damaged nipples. But in most cases, they are a band-aid solution that doesn’t address the root cause of breastfeeding challenges. Instead of reaching for a shield, it’s essential to figure out why the latch is painful or ineffective.
What the Munchkin Nipple Shield Claims to Do
The shield has a “channel” that allows you to see the milk “flowing”—essentially if there is milk in the shield then you will see it go through the little outer channel.
Munchkin’s new design boasts features like:
✔️ A unique cutout to maintain skin-to-skin contact
✔️ A soft silicone material for comfort
✔️ An “optimal” shape for better latch assistance
✔️ Nurse confidently knowing your milk is flowing
Sounds great in theory, right? But here’s the problem—no artificial product can replace the natural skin-to-skin connection, and many nipple shields (even well-designed ones) can interfere with milk transfer, reduce milk supply over time, and make weaning from them difficult.
Why You Don’t Need It
1. Babies Are Born to Breastfeed – Your baby instinctively knows how to find and latch onto the breast. When given the right support—like frequent skin-to-skin contact and an unhurried environment—most babies can latch without any artificial barriers.
2. Pain Is a Sign That Something Needs to Be Adjusted – Instead of masking discomfort with a shield, work with a lactation consultant to fine-tune positioning and latch. Minor adjustments often make a world of difference.
3. Nipple Shields Can Impact Milk Supply – Because they create a barrier between your baby and your nipple, shields can sometimes result in less effective milk removal, which may lead to a drop in supply.
4. Breastfeeding Confidence Comes From Trusting Yourself – The more you rely on your body and your baby’s natural instincts, the more empowered you’ll feel. You don’t need a piece of silicone to tell you that you’re doing it right.
What to Do Instead of Using a Nipple Shield
• Seek professional support – A lactation consultant can help assess latch issues, positioning, and any underlying challenges.
• Try the laid-back breastfeeding position – This allows your baby to use their natural reflexes to latch deeply.
• Give yourself grace – Breastfeeding is a learning process for both you and your baby. Trust that your body knows what to do.
• If you truly do need a nipple shield, this one is not worse than other options, however again I encourage you to trust all the other signs that your baby is getting what they need and not rely on actually seeing the milk in the channel.
Final Thoughts: Less Is More
Moms are already overwhelmed with products that claim to make breastfeeding “easier.” But often, these gadgets create more dependency and self-doubt. The truth? You don’t need a nipple shield unless a trained professional has determined it’s necessary for a specific medical reason. Trust your body. Trust your baby. You’ve got this.
If you’re struggling with breastfeeding and need support, I offer virtual lactation consulting to help you find natural, lasting solutions—without unnecessary interventions. Reach out, and let’s get you and your baby back to basics.
Common Baby Skin Issues and How to Treat Them
A baby’s skin is delicate, soft, and highly sensitive, making it prone to various skin issues. As a parent, it’s natural to worry when you notice rashes, dryness, or other skin concerns on your little one. The good news is that most baby skin issues are harmless and easily treatable. Here’s a guide to some of the most common skin conditions in infants and how to care for them.
1. Diaper Rash
What it is: Red, irritated skin in the diaper area, often caused by prolonged exposure to moisture, friction, or sensitivity to wipes or diapers.
How to treat it:
Change diapers frequently and allow the area to dry before putting on a new one.
Use a diaper rash cream with zinc oxide to protect the skin.
Let your baby go diaper-free for short periods to promote healing.
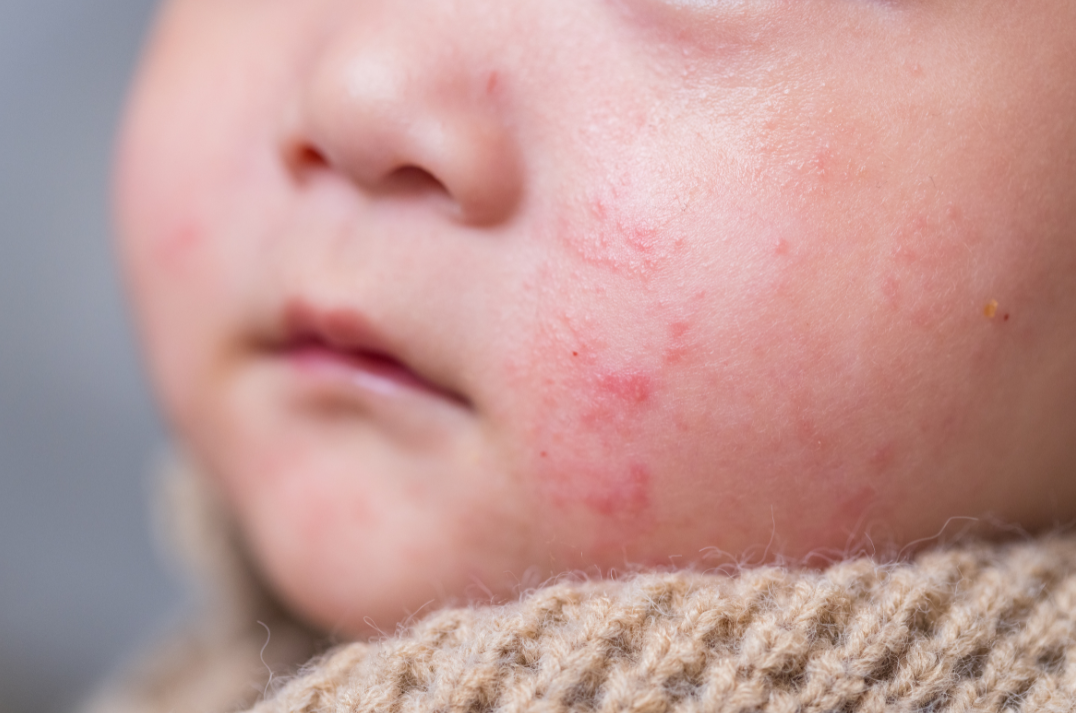
2. Baby Acne
What it is: Small red or white bumps on the face, usually appearing in the first few weeks after birth due to maternal hormones.
How to treat it:
Gently cleanse the face with warm water and a mild baby wash.
Avoid using lotions or oils on the affected area.
Be patient—baby acne usually clears up on its own within a few weeks.
3. Eczema (Atopic Dermatitis)
What it is: Dry, red, itchy patches, often appearing on the cheeks, arms, and legs. Eczema can be triggered by allergens, heat, or irritants.
How to treat it:
Use fragrance-free, hypoallergenic baby lotions and creams.
Dress your baby in soft, breathable fabrics like cotton.
Avoid long, hot baths and use a gentle, soap-free cleanser.
4. Cradle Cap (Seborrheic Dermatitis)
What it is: Scaly, yellowish patches on the scalp, caused by excess oil production.
How to treat it:
Gently massage the scalp with baby oil or coconut oil, then use a soft brush to remove flakes.
Wash your baby’s hair with a mild baby shampoo a few times a week.
5. Heat Rash
What it is: Tiny red bumps that develop in hot, humid conditions when sweat gets trapped in the skin’s pores.
How to treat it:
Dress your baby in loose, lightweight clothing.
Keep them in a cool, well-ventilated area.
Use a cool, damp washcloth to soothe irritated skin.
6. Milia
What it is: Tiny white bumps on the nose, chin, or cheeks caused by blocked skin pores.
How to treat it:
No treatment is needed—milia will disappear on their own as the skin matures.
Avoid picking or scrubbing the bumps.
7. Hives
What it is: Raised, red, itchy welts caused by allergic reactions to foods, insect bites, or environmental triggers.
How to treat it:
Identify and remove the potential allergen.
Apply a cool compress to relieve itching.
Consult your pediatrician if hives persist or cause difficulty breathing.
When to Call a Doctor
Most baby skin conditions are harmless and resolve with gentle care, but seek medical advice if:
A rash is spreading rapidly, oozing, or accompanied by fever.
Your baby seems uncomfortable, fussy, or in pain.
You notice signs of infection (redness, swelling, or pus).
Keeping your baby’s skin healthy involves gentle cleansing, hydration, and avoiding harsh products. If you’re ever in doubt, consult a pediatrician or a baby skin specialist for guidance.
Why Your Pumping Output May Vary: Understanding the Factors at Play
As a breastfeeding mother, you might find that your pumping output fluctuates from day to day, or even from session to session. It can be frustrating and stressful when you don’t seem to be producing as much milk as you expect. While pumping can be a reliable way to express milk, there are a variety of factors that can influence your output. Understanding the reasons behind these fluctuations can help reduce stress and allow you to approach pumping with more confidence. Here are some common reasons why your pumping output may vary.
1. Time of Day
Your milk supply naturally fluctuates throughout the day due to hormonal changes. Many moms find that they produce more milk in the morning, as prolactin—the hormone responsible for milk production—tends to be higher during these hours. On the other hand, milk supply may decrease later in the day as the body starts to wind down. If you notice a drop in your pumping output in the afternoon or evening, it may simply be due to this natural rhythm. Fun fact—your milk is fattier in the afternoon and evening, so although it may be lower volume, it’s still amazing for your baby and made to fill them up for a good sleep.
2. Hydration Levels
Staying hydrated is essential for maintaining a healthy milk supply. Dehydration can lead to a decrease in milk production, and even mild dehydration may affect the amount of milk you can pump. Be sure to drink plenty of water throughout the day, especially before and during pumping sessions. If you find your output is lower than usual, try increasing your water intake and see if it makes a difference.
3. Stress and Anxiety
Stress can have a significant impact on milk production. When you're stressed or anxious, your body releases cortisol, a hormone that can interfere with milk letdown. If you’re feeling stressed about pumping or worried about your milk supply, it’s important to address those feelings. Take deep breaths, practice relaxation techniques, or take a few moments for self-care before pumping to help reduce stress and improve milk flow.
4. Pumping Technique
The way you pump can directly impact your milk output. If you’re using a pump that isn’t the right fit for your body or if you’re not using the proper settings, it could be limiting your milk production. Ensure your flange size is correct (too small or too large can hinder milk flow), and experiment with different suction and speed settings to find what works best for you. Regularly checking your pump’s parts and replacing worn-out components, such as valves and membranes, is also important for maintaining optimal performance.
5. Frequency and Duration of Pumping
Milk production works on a supply-and-demand basis, which means that the more frequently you pump, the more milk your body will produce. If you’ve been pumping less often or for shorter sessions, you might notice a decrease in your output. Increasing the frequency and duration of your pumping sessions can help stimulate your milk supply, especially if you're trying to build up a stash. Make sure you’re pumping long enough to fully empty your breasts, as this encourages your body to make more milk.
6. Diet and Nutrition
What you eat can also influence your milk production. A well-balanced diet rich in nutrients, vitamins, and minerals is essential for maintaining a healthy milk supply. If your diet is lacking in key nutrients, you may notice a dip in your pumping output. Foods such as oats, fenugreek, and flaxseed are often cited as natural galactagogues (substances that help increase milk supply), but it's important to maintain a varied and nutrient-dense diet overall.
7. Fatigue and Sleep Quality
Lack of sleep and exhaustion can impact your milk supply. When you’re tired, your body may not be able to produce as much milk. Sleep is crucial for hormone regulation, and when you’re well-rested, your body can better respond to your baby’s needs or to pumping sessions. While getting enough sleep as a new mom can be challenging, try to rest when you can and avoid pushing yourself too hard.
8. Hormonal Fluctuations
Hormones play a crucial role in breastfeeding, and hormonal changes can affect milk production. For example, your milk supply may dip when you’re about to get your period or during ovulation. Hormonal shifts after childbirth, especially in the early months, can also cause fluctuations in supply. If you’re nearing the end of your maternity leave or considering weaning, you might notice a gradual decrease in milk production as your body adjusts to changes in hormone levels.
9. Illness or Health Issues
Being unwell or experiencing health issues can impact your milk supply. When you’re sick, your body is focused on healing, and milk production may take a temporary backseat. Certain medications, such as those used to treat infections or other conditions, can also impact milk supply. If you’re feeling unwell or taking new medications, it’s worth checking in with your healthcare provider to ensure that your milk production is not being affected.
10. Your Baby’s Needs
Your baby’s feeding habits and growth patterns can also play a role in your pumping output. As your baby grows, they may become more efficient at breastfeeding, meaning they may not need as much milk from you during pumping sessions. Alternatively, if your baby is going through a growth spurt and feeding more frequently, you might experience a temporary drop in pumping output as your body adjusts to meet their increased needs.
11. The Type of Pump
The type of pump you use can also affect how much milk you can express. Manual pumps tend to have lower output compared to electric or hospital-grade pumps, which are designed for higher efficiency. If you’re using a manual pump or a less powerful model, you may find that your output is lower. Hospital-grade pumps are the gold standard when it comes to pumping efficiency, so if you’re concerned about your output, it might be worth considering upgrading to a stronger pump.
12. Emotional Connection to Pumping
Finally, your emotional state can have an impact on your pumping output. Many women find that they produce more milk when they are relaxed and focused on bonding with their baby. If you're distracted, feeling frustrated, or disconnected during pumping sessions, it may be harder to achieve a letdown. Consider looking at photos of your baby or playing a soothing playlist to help encourage your body to produce milk.
Conclusion
Pumping output can vary for many reasons, and it’s important to remember that fluctuations are completely normal. The key is to stay patient and kind to yourself. Rather than stressing over occasional dips in supply, focus on creating a routine that supports your body and its milk-producing capabilities. If you're concerned about your milk supply or if the fluctuations persist, don’t hesitate to reach out to a lactation consultant for personalized support.
Ultimately, your body is doing an incredible job providing nourishment for your baby. Trust in the process and give yourself grace—after all, being a mom is a journey, and every step counts.
Celebrating IBCLC Day: Honoring the Lifesaving Work of Lactation Consultants
Every year, on the first Wednesday of March, we celebrate International Board Certified Lactation Consultant (IBCLC) Day—a day dedicated to recognizing the invaluable contributions of lactation consultants to the health and well-being of mothers and babies around the world. IBCLCs play a crucial role in supporting families on their breastfeeding journey, and today, we take a moment to acknowledge the profound impact they have on communities everywhere.
What is IBCLC Day?
IBCLC Day, celebrated on March 5th this year, is a global observance that highlights the importance of the International Board Certified Lactation Consultant (IBCLC) certification. The day serves as an opportunity to honor these healthcare professionals who are expertly trained to support breastfeeding mothers, address breastfeeding challenges, and promote infant nutrition. The day also serves to raise awareness about the benefits of breastfeeding and the need for skilled support throughout the early stages of parenthood.
Why is IBCLC Day Important?
Lactation consultants are more than just advisors; they are often the key to a successful breastfeeding experience. Their expertise goes far beyond simply teaching breastfeeding techniques. IBCLCs offer personalized support for a variety of breastfeeding-related issues, such as:
Latching and positioning problems
Painful breastfeeding experiences
Low milk supply or overproduction
Breastfeeding after surgery or medical challenges
Breastfeeding twins or multiples
These professionals are trained to assess and provide solutions to any challenge a breastfeeding mother may face. With their support, countless parents are empowered to continue breastfeeding and to bond with their babies in ways that promote both physical and emotional health.
The Journey to Becoming an IBCLC
Becoming an IBCLC requires rigorous training and experience. Lactation consultants must complete extensive coursework in areas such as maternal and infant health, breastfeeding science, human lactation, and medical care, as well as gain hands-on experience through clinical practice. After meeting all the requirements, they must pass the board certification exam, which is internationally recognized.
The path to becoming an IBCLC is demanding, and it reflects the high level of expertise and commitment required to serve families effectively. This certification ensures that IBCLCs have the knowledge and skills to support breastfeeding in the most comprehensive way possible, providing critical care to mothers and babies who may be facing complex breastfeeding issues.
The Lifesaving Role of IBCLCs
The role of an IBCLC goes beyond just guidance; it can truly be life-saving. Studies have shown that proper breastfeeding support, particularly during the early days after birth, can make a significant difference in a mother’s ability to successfully breastfeed. Support from an IBCLC is associated with higher breastfeeding rates, reduced instances of infant health complications, and improved maternal mental health.
For mothers experiencing difficulties with breastfeeding—whether they’re struggling with low milk supply, dealing with painful breastfeeding, or facing a range of other issues—an IBCLC is often the key to resolving those challenges. Their expertise in troubleshooting and problem-solving helps families feel confident and supported, ensuring that babies receive the nourishment they need to grow and thrive.
How IBCLC Day Impacts Communities
On IBCLC Day, communities come together to celebrate the hard work of these dedicated professionals. Hospitals, clinics, and other healthcare settings may host special events, offer educational resources, or provide discounts on lactation services. Social media campaigns raise awareness about the role of IBCLCs and provide resources to new and expectant parents.
IBCLC Day also serves as a reminder to policymakers and healthcare providers of the importance of breastfeeding support in maternal and infant health. By raising awareness about the value of IBCLCs, this day helps ensure that lactation consultants continue to be recognized as vital members of the healthcare team and that more families have access to their life-changing expertise.
How You Can Celebrate IBCLC Day
Thank an IBCLC – If you’ve ever worked with a lactation consultant, take a moment to send them a message of appreciation. Their work has likely made a significant impact on your breastfeeding journey.
Spread Awareness – Use social media to share information about the importance of lactation consultants and their role in supporting breastfeeding. Tag your local IBCLCs or organizations that offer lactation services.
Support Lactation Services – If you’re a healthcare provider or involved in a community organization, consider increasing your support for lactation services. Offer to sponsor an event or provide resources to families in need.
Educate Yourself – Take time to learn more about the benefits of breastfeeding and the expertise of IBCLCs. Understanding the science behind breastfeeding can help you advocate for better support in your own community.
Conclusion
IBCLC Day is a celebration of dedication, expertise, and compassion. It’s a day to honor the hardworking lactation consultants who make a difference in the lives of families across the globe. These professionals provide essential support that not only helps babies thrive but also empowers mothers to nourish and bond with their children in the most meaningful way possible.
So, on March 5th, let’s come together to celebrate IBCLC Day, thank our lactation consultants, and raise awareness about the importance of breastfeeding support. It’s time to shine a well-deserved spotlight on the life-saving work of IBCLCs and ensure that all families have access to the guidance they need to thrive.
Breastfeeding Essentials: What to Buy Before Baby Arrives
Looking for an online birth class? Check out givingbirthnaturally.com
If you’re planning to breastfeed, preparing ahead of time can make the transition smoother for both you and your baby. While breastfeeding is a natural process, it can come with challenges, and having the right tools can help support your comfort and success.
To help you feel ready, here’s a list of breastfeeding essentials to have on hand before your little one arrives.
1. A Comfortable Nursing Bra
Your breasts will change in size throughout your breastfeeding journey, so investing in a few supportive, soft nursing bras is a must. Look for:
Stretchy, wire-free designs that accommodate size fluctuations.
Clip-down or pull-aside styles for easy access.
Breathable, comfortable fabrics to wear day and night. I highly recommend cotton over polyester and other synthetic fabrics
2. Nursing Pads
Leaking is common, especially in the early weeks as your supply regulates. Nursing pads help keep your clothes dry and comfortable. You can choose between:
Disposable nursing pads - Convenient and absorbent for on-the-go.
Reusable nursing pads - Eco-friendly and soft against the skin.
3. Nipple Cream
Sore or cracked nipples can occur as you and your baby adjust to breastfeeding. A good nipple cream provides relief and helps with healing. Look for:
Lanolin-based creams or natural alternatives like coconut oil.
Products that are safe for baby and don’t require wiping off before nursing.
4. A High-Quality Breast Pump
Even if you plan to exclusively breastfeed, having a breast pump can be helpful for:
Building a freezer stash.
Relieving engorgement.
Allowing your partner or other caregivers to help with feeds.
Types of breast pumps to consider:
Electric pumps - Great for regular pumping, especially if you plan to return to work.
Manual pumps - Simple, portable, and useful for occasional pumping or relieving engorgement.
Wearable pumps - Hands-free and discreet, ideal for multitasking.
Many insurance plans cover breast pumps, so check with your provider before purchasing one!
5. Milk Storage Bags or Containers
If you plan to pump, you’ll need a way to store breast milk. Breast milk storage bags are:
Pre-sterilized and easy to freeze.
Designed to lay flat for efficient storage.
You can also use BPA-free storage bottles if you prefer to store milk in the fridge.
6. A Nursing Pillow
A supportive nursing pillow helps position your baby at the right height, reducing strain on your arms, neck, and back. Consider:
A C-shaped pillow for classic nursing positions.
A firmer pillow for extra support (great for C-section recovery).
7. Breastfeeding-Friendly Clothing
Having a few nursing-friendly tops, pajamas, or dresses makes feeding easier, especially in the early days. Look for:
Tops with pull-down or button-front access.
Loose, comfortable fabrics that allow for skin-to-skin contact.
8. A Water Bottle and Snacks
Breastfeeding is thirsty work! Keeping a large water bottle nearby helps you stay hydrated. Having easy-to-grab snacks like nuts, protein bars, or fruit can also keep your energy up during long nursing sessions.
9. Lactation Support Items (If Needed)
Some moms find that lactation teas, cookies, or supplements help with milk supply. While not essential for everyone, they can be useful if you experience supply concerns.
10. A Lactation Consultant’s Contact Information
One of the best ways to set yourself up for breastfeeding success is to know where to turn for help if needed. A lactation consultant can assist with:
Proper latch and positioning.
Engorgement or clogged ducts.
Low milk supply concerns.
At Mama Milk, we offer virtual lactation consultations and in-person support to help you and your baby thrive on your breastfeeding journey.
Final Thoughts
Having these essentials ready before your baby arrives can help you feel confident and prepared for breastfeeding. While every journey is different, support and the right tools can make all the difference.
Need help with breastfeeding? Mama Milk is here for you! Contact us for lactation support, craniosacral therapy, and more.